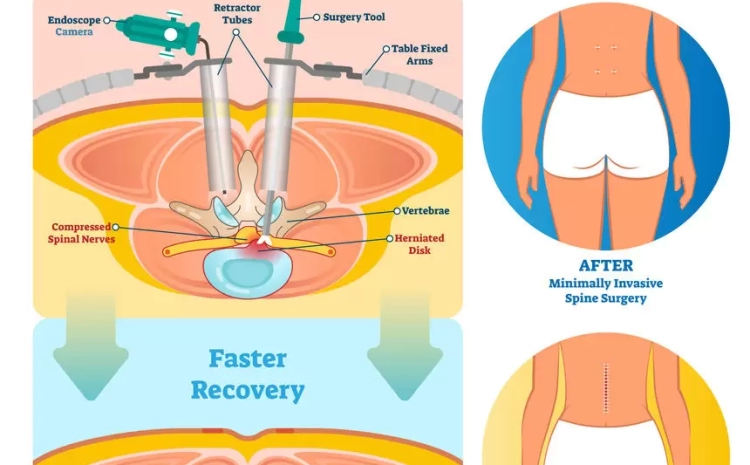
Back and spine ailments are among the most common diagnoses worldwide. Millions suffer everyday from persistent lower back pain, slipped discs, and spinal stenosis, limiting mobility and quality of life. Spine surgery was once considered a last resort due to its huge incisions, long hospital stays, and painful rehabilitation. However, minimally invasive spine surgery (MISS) has modified that attitude. Patients can now get accurate, successful spine operations with smaller incisions, less pain, and faster recovery.
Learning Minimally Invasive Spine Surgery
Modern minimally invasive spine surgery treats spinal diseases with minimal muscle, tissue, and bone damage. Most open surgery requires big cuts and muscle retraction to access the spine, while minimally invasive treatments use tiny incisions, specialized equipment, and enhanced imaging to reach the damaged area.
MISS surgeons use microscopic or endoscopic cameras to examine inside the spine for precise surgery. Tissue injury, infection, and blood loss are reduced using this method. Thus, postoperative discomfort is reduced and patients can resume regular activities sooner.
Minimally Invasive Surgery Treats Common Conditions
Minimally invasive methods can cure several spinal problems. These include herniated discs, spinal stenosis, spondylolisthesis, degenerative disc disease, and spinal abnormalities. It stabilizes the spine following fractures and other traumas.
Each of these procedures aims to relieve spinal cord or nerve pressure, rectify alignment difficulties, and restore spinal stability while keeping as much natural anatomy as feasible. Patients seeking an alternative to open back surgery may prefer the technique due to its smaller incisions and less muscle damage.
Minimal Invasive Surgery vs. Traditional Methods
Traditional spine surgery involves big incisions for direct spine access. This entails cutting or tugging muscles and tissues, which increases blood loss, scarring, and recovery time. Minimally invasive surgery combines tubular retractors and micro-instruments to create a narrow working tunnel to access the spine without injuring surrounding structures.
Surgeons can locate damaged vertebrae and nerves using fluoroscopy or intraoperative navigation. High-definition microscopes and endoscopes provide precise, safe motions. After the treatment, the incision, usually a few centimeters long, is healed with few sutures, leaving a minor scar.
Minimally Invasive Spine Surgery Benefits
One of the main reasons minimally invasive spine surgery is so popular is its many advantages over traditional surgery.
Most importantly, patients feel less discomfort. Muscles and soft tissues are not substantially sliced or stretched, therefore recovery is faster and less painful. With many treatments now outpatient, patients can go home the same day, reducing hospital stays.
Faster recuperation is another benefit. While open surgery takes months to heal, most patients can return to light work and regular activities within weeks. Since internal tissues are less exposed, the smaller incision reduces scarring and infection risk.
Blood loss during surgery is considerably minimized, reducing problems and transfusions. Minimally invasive surgeries are safer, more comfortable, and yield superior long-term results.
Technology in Modern Spine Surgery
Without technology, minimally invasive spine surgery is impossible. Computer-assisted navigation, robotic guiding, and advanced imaging technologies make precise and delicate surgeries easier than ever.
3D imaging helps surgeons maneuver around crucial nerves and tissues by visualizing the spine in real time. Robotic-assisted technologies position implants and screws precisely. Even the most intricate surgeries are more controlled and predictable with endoscopic cameras’ clear and magnified views.
These improvements boost surgical outcomes and patient safety. Human skill and technology precision are the future of spine care.
The Patient Experience: Surgery to Recovery
Minimally invasive spine surgery is often less intimidating than expected. MRIs and CT scans are used to identify the condition before surgery. It takes less time than traditional surgery and is done under general anesthesia.
Patients should move as quickly as feasible after surgery, sometimes within hours. Mild drugs treat pain, and stiffness and discomfort are minor because muscles are mostly intact. Most patients are discharged in one or two days and can resume modest activities.
Many people see great mobility and pain reduction within weeks. Back muscles and posture may be strengthened with physical therapy throughout rehabilitation. Rehabilitation is easier, faster, and less demanding than open surgery.
Who Can Have Minimally Invasive Spine Surgery?
Not all spinal diseases can be treated minimally invasively, but many can. This method benefits ruptured discs, sciatica, degenerative spinal changes, and spinal stenosis patients.
Your neurosurgeon will assess your symptoms, imaging, and health before recommending the procedure. Traditional open surgery may be needed in difficult patients with multiple spinal anomalies or severe deformities. For most regular spinal disorders, minimally invasive treatments yield great solutions with less risks.
Why You Need an Experienced Neurosurgeon
Although minimally invasive spine surgery sounds easier, it needs precision, expertise, and experience. A skilled neurosurgeon with modern spinal methods is essential for safety and success. Experienced surgeons can determine which patients will benefit most from the surgery and tailor treatment programs.
A skilled neurosurgeon will coordinate preoperative, postoperative, and long-term therapy. Their knowledge guarantees that you receive surgical and holistic care that treats the fundamental cause of your discomfort and prevents future issues.
Life After MI Spine Surgery
Recovery after minimally invasive spine surgery is usually smooth and enjoyable. Patients often receive pain relief and mobility improvements within days following the surgery. They can gradually resume normal habits and even unpleasant physical activities as the spine recovers.
Living a healthy lifestyle following surgery is crucial to maintaining benefits. Regular exercise, healthy posture, weight management, and ergonomics can prevent spine problems. Optimal care and medical follow-up can make minimally invasive spine surgery a lifetime advantage.
Conclusion
One of the greatest medical advances is minimally invasive spine surgery. It is safer, faster, and less painful than traditional spine surgery because to surgical precision and cutting-edge technology. Patients might now see substantial back pain treatment without the extensive recovery times of spine procedures.
Consulting a qualified neurosurgeon about minimally invasive treatments may help chronic spine patients regain movement, comfort, and confidence. This method redefines healing—gently, effectively, and with fresh freedom—with less incisions and bigger benefits.




