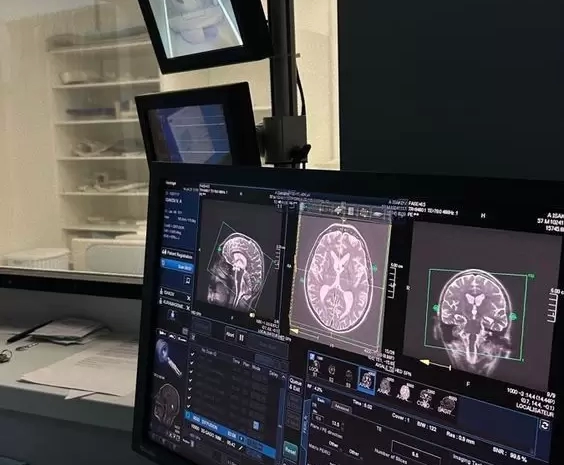
Long considered one of the most delicate medical areas, brain surgery. The brain controls movement, memory, emotions, and all thoughts. For decades, operating on such a sensitive organ carried severe dangers during and after operation. The latest medical technology makes brain surgery safer, more precise, and less intrusive than ever.
Innovation defines modern neurosurgery. High-definition imaging, computer-assisted navigation, robotics, and AI are changing surgery. These devices save lives, speed recovery, reduce problems, and improve patient outcomes.
Brain Surgery Evolution
In the beginning of neurosurgery, brain surgeries were dangerous and performed without much knowledge about brain function. Surgeons used external cues, anatomical knowledge, and physical expertise to find issues without modern imaging. This made surgeries risky and prolonged, increasing the risk of infections, bleeding, and function loss.
Continuous research and technical advances have transformed the sector in recent decades. Once high-risk procedures are now conducted with unprecedented precision. Contemporary neurosurgeons can map the brain, view it in real time, and undertake delicate procedures through tiny incisions. After saving lives, the focus is now quality of life.
The Power of Advanced Imaging
Safer brain surgeries start with modern imaging. CT and MRI scans have changed how surgeons view the brain before and during surgery. Neurosurgeons can locate tumors, blood clots, and damaged tissues using high-resolution 3D images.
Brain activity mapping is added to functional MRI (fMRI). Surgeons can avoid important areas by seeing which brain regions govern movement, speech, vision, and emotion. Diffusion Tensor Imaging (DTI) helps select surgical paths that maintain neural connections by visualizing nerve fiber patterns.
MRI and CT imaging during surgery have increased safety. The real-time imaging help surgeons to determine that the tumor or lesion was entirely removed without injuring adjacent tissue. This greatly reduces the chance of incomplete removal or additional procedures.
Neuronavigation: Brain GPS
Precision in neurosurgery is difficult. A millimeter’s variation can disrupt vital brain functioning. Neuronavigation technologies, or “GPS for the brain,” have improved surgical accuracy. Computer-guided systems produce 3D brain maps using preoperative imaging data.
The neurosurgeon can track surgical instruments on a screen during surgery using this map. Neuronavigation helps surgeons find the problem, much a GPS helps drivers. Avoiding key locations, reducing incision size, and protecting healthy brain tissue are benefits.
Precision has greatly improved tumor removal and epilepsy surgery outcomes. Patients heal faster, have fewer problems, and preserve neurological function.
Increasing Minimally Invasive Neurosurgery
Traditional brain procedures involved big incisions and skull removal, which increased infection risk and recuperation time. Neurosurgeons can now undertake minimally invasive treatments that are less stressful with new instruments and imaging systems.
In endoscopic brain surgery, a tiny tube holds a camera and surgical equipment. To reach deep brain locations, this gadget is placed through small skull apertures or the nose. The surgeon uses specialized equipment to move precisely while viewing a high-definition image of the surgical site on a monitor.
These methods reduce pain, scarring, and hospital stays by using smaller holes. They can often resume typical routines in weeks rather than months.
Robotic Neurosurgery
Neurosurgery has been transformed by robotic-assisted surgery. Human hands cannot match robot precision and stability. They conduct precise movements so well that they reduce human mistake and tiredness throughout extended processes.
The surgeon uses a console to guide robotic arms with real-time image feedback in robotic neurosurgery. The robot’s smooth, regulated movements aid delicate procedures like tumor biopsies and deep brain stimulation.
Electrodes in specific brain locations are used in deep brain stimulation to treat Parkinson’s disease. Robots accurately implant these electrodes, boosting outcomes and lowering adverse effects. Robotics improve precision, predictability, and efficiency in difficult surgeries.
Machine Learning and AI in Brain Surgery
AI is becoming more significant in neurosurgery. AI technologies can help surgeons plan treatments, identify hazards, and make better judgments by evaluating massive patient data.
Machine learning algorithms can spot brain scan patterns that humans cannot. They can differentiate good and abnormal tissue, help surgeons access tumors safely, and help diagnose brain problems earlier.
Additionally, AI-powered platforms improve intraoperative monitoring. They monitor brain activity, blood flow, and pressure in real time to notify the surgery team to potential issues. Brain surgery will become more accurate and safe as these technologies advance.
3D Printing in Neurosurgery
Neurosurgery takes advantage of 3D printing. From CT or MRI data, surgeons may develop precise, patient-specific skull and brain models. These models improve surgeon planning and practice of complex surgeries before surgery.
In other circumstances, 3D-printed implants rebuild skull sections removed during surgery. These bespoke implants improve safety and cosmetics by fitting correctly. Personalized care enhances surgical precision and patient confidence in therapy.
Live Intraoperative Monitoring and Feedback
Brain function must be monitored during brain surgery. Intraoperative neurophysiological monitoring lets doctors see brain activity during surgery. Electrodes on the scalp or brain surface monitor electrical activity, protecting movement, speech, and vision.
This real-time feedback lets neurosurgeons change their strategy immediately if the data suggests brain damage. It protects against postoperative consequences like paralysis, speech problems, and memory loss.
Ultrasonic and Laser Technology
Lasers and ultrasonic tools are increasingly employed in neurosurgery to remove tissue precisely. Instead of damaging surrounding tissues, laser ablation employs focused light to remove tumors or aberrant tissues. By using small holes, these techniques can reduce damage and expedite recuperation.
Ultrasonic aspirators softly break down and remove tissue using vibrations. Both methods are useful for treating deep-seated tumors and epilepsy-related brain disorders where surgery is too dangerous.
Brain Surgery Future: VR and Beyond
Brain surgery will increasingly use digital and virtual technologies. VR and AR are used to simulate procedures, train clinicians, and visualize brain anatomy in 3D. These tools let surgeons practice and predict problems before operating on patients.
Augmented reality gives surgeons a better picture of anatomy during procedures. This real-time visualization boosts accuracy and lowers uncertainty. As these technologies improve, brain surgery planning and execution will be closer.
How These Advances Help Patients
All these technology advances aim to improve patient safety and outcomes. Modern neurosurgeries are less intrusive, more accurate, and faster to recover. Lower infection rates, shorter hospital stays, and greater brain function are achieved.
The psychological impact of surgery has also decreased. Patients and families are more confident when they know operations are safe and successful. Patient care is compassionate and cutting-edge thanks to human expertise and innovative technology.
New Precision and Hope Era
Neurosurgery is medically innovative. A once-risky enterprise is now a precise and controlled science. From imaging and robots to AI, each technological innovation takes brain surgery closer to a safer, more rewarding future.
Neurosurgeon talent and judgment drive this improvement. While technology provides tools, human expertise guides them with care and compassion. They collaborate to push contemporary medicine forward.
Brain surgery will becoming safer, smarter, and more successful as technology develops. This offers neurological patients a shot at survival and a better, fuller life.




